What came first, the chicken or the egg? Hi, I’m Josie Gannon. I’m a board certified clinical specialist in pediatric physical therapy. I’m going to talk to you about a different form of this question. What came first, the flat spot or the tight neck. One of the most common reasons infants are referred to physical therapy is due to a developing flat spot on their head (plagiocephaly) and/or a tight neck (torticollis). I wanted to explain why we should be looking for it right away, what to do if you notice either scenario, and the long term consequences.
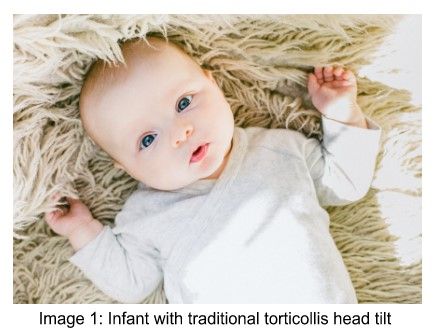
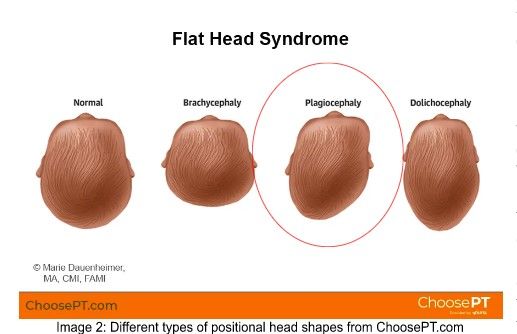
First, let’s talk about what these terms mean. Torticollis is a postural deformity evident shortly after birth, typically characterized by lateral flexion of the head and contralateral rotation due to unilateral shortening of the sternocleidomastoid (like Image 1). Plagiocephaly is a flat spot on the posterolateral aspect of the head as seen in image 2.
Why is early identification of either situation important? For torticollis, research demonstrates that duration of treatment is correlated with how early a child starts physical therapy. It’s ideal for us to see an infant before or by 3 months. This is for various reasons, but I’ll tell you the two that stand out the most. First of all, research specifically says, starting physical therapy by 3 months averages about 3 months of therapy. Starting between 3 to 6 months averages 6 months of physical therapy. Your time is precious. Driving to and from a clinic 1 time a week, during business hours, is not ideal. Second, before 3 months, they don’t quite have full head control. This allows parents to complete a more passive home exercise program. As infants gain strength and motor control, they want to visually or physically explore their environment. What does that mean for us? Finding engaging ways to complete their stretches and strength exercises is harder for their therapist and their parents. We typically recommend that these exercises are performed each diaper change. Once they are strong and independent, this can make diaper changes tedious, requiring parents to find other times in the day to make it work. Beyond time in therapy, torticollis can also result in delayed gross motor skills because your child does not have balanced trunk and neck musculature. This makes balance much more difficult.
When we talk about a flat spot, early identification also makes things easier on you. For a flat spot, we preach repositioning. So it makes sense that the less they move, the easier it is to correct head shape. When repositioning is initiated before baby is rolling, it is much simpler to avoid a helmet. If a helmet is prescribed, it is an orthosis worn 23 hours per day. Typically, at least 2 months of therapy is suggested prior to ordering a custom helmet.
How can you look out for these things at home? PICTURES! I know you have a million photos of that sweet munchkin on your phone. Do they always have their head tilted to the same side (like in Image 1)? Do they only turn their head one direction? These are signs of a tight neck. See if they can visually track a toy through the same range in both directions. Often this task is difficult when torticollis is present. Flat spots can also be identified with pictures. Hold baby so someone can take a picture of the top of their head (like Image 2). If they have thick hair, take the picture after bathtime. You can use these images to not only identify if there’s a flat spot, but also to monitor changes.
So you think your little one has torticollis or plagiocephaly, what now? It’s time to come visit a PT! Depending on your insurance you may or may not need a referral from your primary care provider. I recommend discussing your concerns with them right away regardless. Remember our job as healthcare providers is to provide you with the facts to make an educated decision. It’s ok to ask for a referral rather than waiting for someone else to bring it up. In my experience, treatment can last anywhere from 2 sessions to a year. Of course, you can look online for solutions to this issue, but physical therapists are trained to screen for other underlying issues that may be contributing such as vision, neurological, and musculoskeletal impairments. If something else is causing baby to rotate or tilt to one side, traditional stretches and exercises won’t have the same effect. We also have ways to modify the typical stretches and exercises to make them more comfortable for you and baby. Remember, that nothing should be added to your child’s crib or car seat to correct their head position unless it has been approved or crash tested. Safety first!
Now let’s talk about the consequences of torticollis and plagiocephaly. Why is it important to correct? Torticollis holds an infant’s head in rotation and a lateral tilt. When baby is learning to complete new motor milestones they need to learn to complete them both directions for symmetrical strength. If they are only looking one way, they often learn to complete skills in only one direction. This is a combination of them using vision and compensating for having a weak neck muscle on one side. Plagiocephaly allows them to rest more to their preferred side. This makes addressing their torticollis more difficult. Evidence states that it is mainly cosmetic, meaning there are visible asymmetries (flat spot, asymmetrical ears, asymmetrical eyes, ect), but no long term consequences (no it’s not pushing on your child’s brain).
Here’s the bottom line, many things can contribute to a flat spot (plagiocephaly) or tight neck (torticollis). Don’t get down on yourself if you or your pediatrician notice one. Instead focus on tackling this head on. We know this should be addressed as early as possible for a couple reasons. The main ones being, early treatment decreases the time in physical therapy and decreases the odds of asymmetrical development. Treatment is guided by a physical therapist, but a majority of the work is completed by parents at home. If there is anything you take from this article, I want you to feel empowered to identify torticollis or plagiocephaly early, so you can advocate for your child to receive prompt treatment.
Catch ya later!
Josie Gannon, PT, DPT
Board Certified Clinical Specialist in Pediatric PT
Instagram: @peds_perspective